
Arteries and Veins: Structure, Classification, and Organ Features
A detailed exploration of blood vessel distinctions and functional histological features
Key Highlights
- Structural Layers: Both arteries and veins share a three-layered structure—tunica intima, tunica media, and tunica adventitia/externa—but vary considerably in thickness and composition.
- Classification Nuances: Arteries include elastic and muscular types based on elasticity and smooth muscle content, while veins are categorized by size and location with notable features like valves.
- Histological and Organ Features: Arteries are designed to handle high pressure from the heart, and veins possess larger lumens and valves that aid in returning blood, with specialized systems such as the portal vein integral to hepatic function.
Introduction
The human circulatory system is a complex network that maintains sustained blood flow throughout the body. Central to this system are blood vessels, which are divided into arteries, veins, and capillaries. This discussion provides an in-depth analysis of arteries and veins, focusing on their source and structure, classification, histology, and organ-specific features—particularly the structural nuances of veins. Understanding these differences is crucial for comprehending how blood is transported, how pressure is managed, and how the body adapts to varying physiological demands.
Artery and Vein: Basic Definitions and Origins
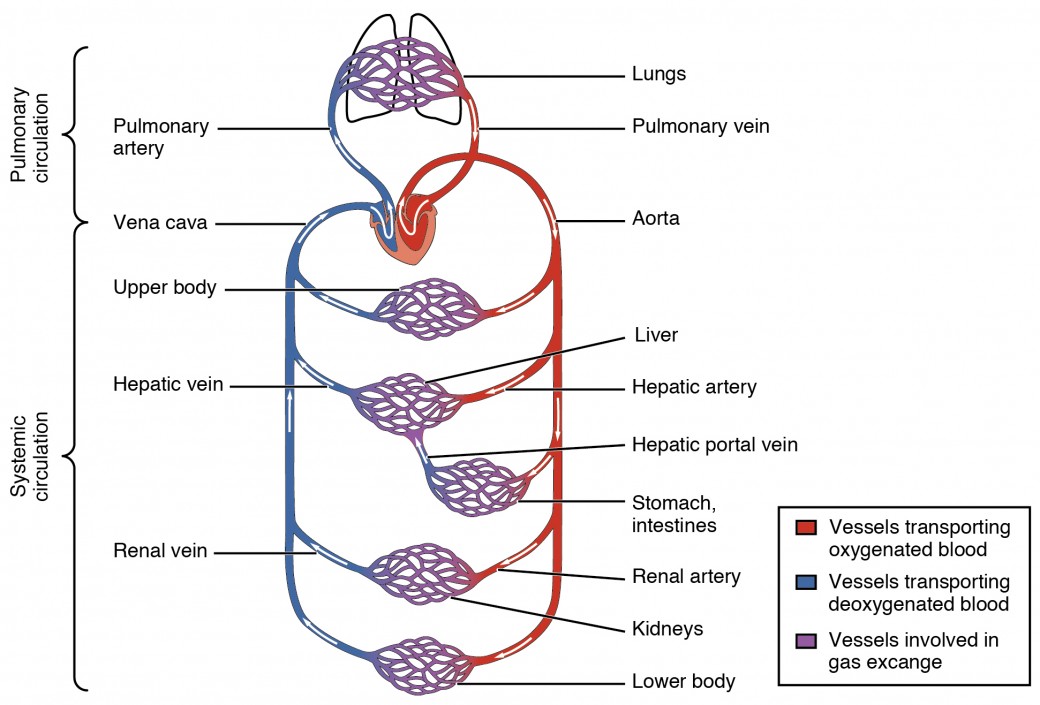
Arteries are blood vessels tasked primarily with conducting oxygen-rich blood away from the heart to the tissues of the body; the pulmonary artery is an important exception as it carries deoxygenated blood to the lungs. In contrast, veins are responsible for returning deoxygenated blood back to the heart, with the pulmonary veins carrying oxygenated blood from the lungs to the heart. This fundamental directional flow supports the effective operation of the cardiovascular system, ensuring that oxygenation and nutrient delivery are maintained.
The sources of these vessels stem embryologically from different regions and undergo specialized development processes. From early differentiation in the cardiovascular mesoderm, the arteries develop thick, muscular and elastic walls to accommodate high pressures. Venous formation, on the other hand, results in thinner-walled, more compliant channels with specialized structures such as venous valves to prevent blood backflow and maintain directional flow, especially under low-pressure conditions.
Structural Organization: Tunics of Blood Vessels
Overview of Vessel Layers
Both arteries and veins are organized into three distinct layers that impact their functional performance:
Tunica Intima
This innermost layer is in direct contact with the blood flow. The tunica intima is composed of a single layer of endothelial cells that provides a smooth surface reducing friction and facilitating laminar flow. In arteries, this layer is often reinforced by an internal elastic lamina, which aids in maintaining elasticity, particularly in vessels closer to the heart.
Tunica Media
The tunica media is the middle layer and comprises mostly smooth muscle cells and elastic fibers. This layer is significantly thicker in arteries than in veins due to the requirement to withstand and modulate the high pressure of blood ejected directly from the heart. In muscular arteries, the smooth muscle content is predominant, enabling precise regulation of vessel diameter through vasoconstriction and vasodilation.
Tunica Adventitia (Externa)
The outermost layer, known as the tunica adventitia or externa, provides structural support and protection. It is comprised predominantly of connective tissue, collagen, and in veins, may be more pronounced than in arteries. This layer not only anchors the vessel to surrounding tissues but also houses smaller blood vessels (vasa vasorum) that supply the vessel walls themselves.
The differences in the thickness and composition of these layers account for the distinct functions of arteries and veins. For example, the thick tunica media in arteries is essential for managing the high and pulsatile pressures from the heart, whereas the thinner tunica media in veins is sufficient for the lower, steady pressures involved in venous return.
Classification by Structure and Function
Arteries: Elastic and Muscular Types
Arteries can be broadly classified into two main types based on their histological characteristics and location in the circulatory system.
Elastic Arteries
Elastic arteries, such as the aorta and pulmonary trunk, are positioned close to the heart. Their walls are rich in elastic fibers, which enable them to stretch in response to the surges of blood pumped from the heart (systole) and recoil during diastole. This elasticity is critical for cushioning the effects of blood pressure fluctuations and ensuring a continuous flow. The high concentration of elastic tissue in these arteries allows them to serve as pressure reservoirs that mitigate the stress on the vascular system as blood is pushed forward.
Muscular Arteries
Positioned further from the heart, muscular arteries contain a lower proportion of elastic fibers and a higher concentration of smooth muscle cells. These arteries, for example, the radial and femoral arteries, are smaller in diameter and play a pivotal role in regulating blood flow to specific organs and tissues through vasoconstriction and vasodilation. This regulation is essential for responding to local metabolic demands, thereby maintaining homeostasis.
Veins: Categorization Based on Size and Location
Veins are generally structured to accommodate large volumes of blood as they return it to the heart. Their classification is often based on their size, anatomical location, and specific physiological roles.
Superficial Veins
Superficial veins lie just beneath the skin, often visible and implicated in thermoregulation. They are less muscular and more variable in terms of structure. Their position makes them subject to external compression, an attribute that is useful in clinical diagnoses such as varicose vein assessments.
Deep Veins
Deep veins are located deeper within muscle tissue, often running alongside arteries. Their closeness to muscular structures enables them to benefit from the "muscle pump" mechanism, where muscle contractions help push blood through these veins.
Pulmonary and Systemic Veins
Pulmonary veins are unique as they convey oxygenated blood from the lungs to the heart, contrasting with the typical role of veins in returning deoxygenated blood. Systemic veins, on the other hand, collect deoxygenated blood from the body, funneling it towards the heart. The distinction between these two types underscores the specialized roles that veins play in different parts of the circulatory loop.
A table summarizing these distinctions is presented below:
| Feature | Arteries | Veins |
|---|---|---|
| Direction of Blood Flow | Away from the heart (except pulmonary artery) | Toward the heart (except pulmonary veins) |
| Wall Thickness | Thicker (due to thicker tunica media) | Thinner (less muscularity in tunica media) |
| Lumen Diameter | Narrower | Wider |
| Presence of Valves | Generally absent | Present, especially in the limbs |
| Blood Pressure | High, pulsatile flow | Low, steady flow |
| Structure of Tunica Media | Rich in smooth muscle and elastic fibers | Less prominent smooth muscle |
Detailed Histology of Arteries and Veins
Histological Architecture
The histological structure of arteries and veins reflects their differing functional requirements. These tissues are best understood by examining their cellular composition and structural differences at the microscopic level.
Arterial Histology
In arteries, the thick tunica media contains layers of smooth muscle cells interspersed with elastic fibers, particularly abundant in elastic arteries. This arrangement permits arteries to withstand high pressure and maintain a consistent flow during the cardiac cycle. The luminal surface is lined by a continuous layer of endothelial cells that reduce friction and help mediate vascular tone. The presence of an internal elastic lamina is a distinctive feature seen especially in large arteries, contributing to their resilience and ability to rebound after each systolic expansion.
The arrangement of collagen and elastin fibers in the arterial wall serves not only to absorb mechanical stress but also to regulate vessel constriction. This balance between elasticity and contractility is crucial for maintaining systemic blood pressure and ensuring efficient blood circulation throughout the body.
Venous Histology
Veins, by contrast, exhibit a thinner tunica media with fewer smooth muscle cells, since the mechanical forces acting upon them are less intense than in arteries. This structural adaptation is complemented by a much larger luminal diameter, offering a capacitance function that accommodates a significant volume of blood. A noteworthy histological feature in many veins is the presence of valves housed within the tunica intima. These valves are essential in preventing backflow and ensuring unidirectional blood movement, particularly in regions where venous pressure is low and gravity may impede blood return, such as in the legs.
The tunica adventitia in veins tends to be more robust than that in arteries, primarily because it compensates for the weaker muscle layer by providing structural support and protection. Additionally, veins are often embedded within connective tissue that anchors them within the body, which further helps maintain their patency under various physiological conditions.
In some specialized venous structures, such as the portal system, unique histological adaptations are evident. The portal vein collects nutrient-rich blood from the gastrointestinal tract and directs it to the liver for detoxification. This system is marked by a network of smaller venules that coalesce into larger veins, reflecting a hierarchy of vessel size and function.
Organ Features and Functional Aspects of Veins
Specialized Venous Systems
The venous system is not homogeneous; it encompasses numerous specialized networks adapted to meet particular physiological demands. The systemic venous system collects deoxygenated blood from the body's tissues, but several subsystems showcase unique features:
Superficial and Deep Veins
Superficial veins are easily visible just beneath the skin and play an important role in regulating body temperature through heat exchange. In contrast, deep veins are found alongside arteries and within the confines of muscle compartments. The proximity of deep veins to muscular contractions promotes the effective return of blood to the heart through the muscle pump mechanism—contractions of surrounding muscles compress the veins, aiding forward blood flow.
The Portal Venous System
The portal vein is a distinctive venous structure that collects blood from the gastrointestinal tract, pancreas, and spleen, and transports it directly to the liver. This system ensures that nutrients and toxins absorbed in the gut are first processed by the liver before the blood recirculates to the heart. This functional feature is critical in metabolic regulation and detoxification, protecting the body from potentially harmful substances.
Cranial and Spinal Venous Networks
The cranial and spinal regions contain a network of veins that manage blood drainage from the brain and spinal cord. These veins have unique anatomical interconnections and are capable of collateral circulation. The absence of valves in certain sections of the venous drainage system creates a network adaptable to changes in intracranial and spinal pressures, which is particularly important in maintaining cerebrospinal fluid dynamics and ensuring adequate venous return even in varied postural conditions.
Functional Importance of Venous Valves
The presence of valves in many veins is one of the most distinctive organ features associated with venous structure. Valves, commonly located in the limbs, function to avert the retrograde flow of blood and are critical in counteracting the effects of gravity when the body is in an upright position. These anatomical structures, by ensuring a unidirectional flow, are fundamental to preventing venous stasis and reducing the risk of conditions such as deep vein thrombosis (DVT).
Additionally, the location and density of veins vary in accordance with physiological necessity. For instance, in areas where gravitational stress is maximal, such as the lower extremities, the prevalence of venous valves is proportionately increased. This strategic anatomical planning underscores the body's natural inclination to optimize blood return and maintain effective cardiovascular circulation.
Integration of Source Insights into a Comprehensive Analysis
The differential characteristics between arteries and veins become evident when comparing both the gross anatomical structure and the histological composition. Arteries, designed for high-pressure and pulsatile blood flow, are inherently built to be strong and resilient. Their thick, muscular, and elastic walls make them capable of withstanding the significant mechanical forces exerted during each heart contraction. Moreover, their classification into elastic and muscular arteries highlights the gradient of function—from cushioning the impact of the heart's pumping action to regulating blood distribution at a more localized level.
Veins, however, are specifically engineered to facilitate the return of blood under much lower pressure conditions. Their structural design emphasizes volume capacity and directional stability rather than pressure tolerance. The larger lumen and the presence of valves contribute to an efficient venous return, even in the presence of gravitational challenges. Additionally, the histological composition, characterized by a thinner tunica media and a relatively thicker tunica adventitia, reflects a shift in functional emphasis—from maintaining a high-pressure environment to ensuring adequate capacity and protection of the vessel.
While both arteries and veins belong to the same vascular family and share similar basic structures, the differences in their histology and functional categorizations are not merely academic. They have significant clinical implications, ranging from the interpretation of vascular diseases to surgical interventions. For example, arterial stiffness is a key factor in hypertension, whereas venous insufficiency is a major contributor to leg swelling and varicose veins. Understanding these nuances is critical for healthcare providers as they diagnose, treat, and manage cardiovascular conditions.
Comparative Analysis: Clinical and Functional Relevance
Clinical Implications of Arterial Histology
The arterial wall's substantial muscular and elastic components make these vessels primary targets in conditions like atherosclerosis, hypertension, and aneurysms. In atherosclerosis, the deposition of plaques compromises the elasticity and contractility of arteries, directly impacting their ability to accommodate changes in pressure. This phenomenon emphasizes the need for therapeutic strategies that improve endothelial function and reduce arterial stiffness.
Clinical Implications of Venous Histology
On the venous side, the structural characteristics such as thin walls and distinct valve architecture predispose these blood vessels to conditions like deep vein thrombosis (DVT) and venous insufficiency. The importance of maintaining unidirectional blood flow through these valves cannot be understated, as their dysfunction may lead to blood pooling and subsequent clot formation. Clinical interventions often focus on improving venous return via compression therapies or surgical correction of defective valves to mitigate such risks.
Moreover, specialized venous systems such as the portal vein have unique clinical significance. For instance, patients with liver cirrhosis often develop portal hypertension, where increased pressure within the portal vein system leads to a cascade of complications including variceal bleeding and ascites. This underscores the importance of understanding venous architecture in both preventive and therapeutic contexts.
Conclusion and Final Thoughts
In summary, the detailed exploration of arteries and veins reveals how their distinct structural, histological, and functional characteristics are finely tuned to their roles within the circulatory system. Arteries, with their robust, multi-layered structure featuring a thick tunica media, are optimized to handle the significant pressures generated by the heart, ensuring the effective delivery of oxygenated blood to critical tissues, while special classifications such as elastic and muscular arteries serve varied functions from shock absorption to localized blood flow regulation.
Venous structures complement this system through their adaptability to low-pressure environments. Their larger lumen, strategic presence of valves, and variations between superficial and deep systems allow for maximal blood volume accommodation and directional control. Organ-specific adaptations, such as those observed in the portal vein system, underscore the complexity and fundamental importance of venous return in metabolic processing and detoxification.
Clinically, both arterial and venous histology play crucial roles in disease manifestation and treatment strategies. Recognizing the nuances inherent in these vascular structures, from the resilient elasticity of arteries to the compliance and valve function of veins, contributes significantly to both diagnostics and the design of therapeutic interventions.
This integrated review not only elucidates the basic anatomical classifications and histological features that differentiate arteries and veins, but it also highlights how these differences are pivotal to maintaining healthy circulatory dynamics. Future research and clinical advancements continue to build upon this foundation, helping improve patient outcomes across a spectrum of cardiovascular conditions.
References
- Blood Vessel Classification - SEER Training
- Histology of the Cardiovascular System - Kenhub
- Artery and Vein Histology - Osmosis
-
Veins Overview - Cleveland Clinic
-
Blood Vessels - Cleveland Clinic
- Circulatory Blood Vessels - Visible Body
- Differences Between Arteries and Veins - WebMD
- Structure and Function of Blood Vessels - Pressbooks
- Blood Vessel - Wikipedia
- Blood Vessel Structure - NCBI Bookshelf
Recommended Further Reading
Last updated February 23, 2025