
Navigating Recovery: Functional Outcomes After a Comminuted Non-Displaced Humeral Fracture in Elderly Patients
Understanding the Path to Healing and Regaining Function in the Upper Arm
A comminuted non-displaced humeral fracture in a 67-year-old woman presents a unique set of considerations for functional outcome, especially given the patient's age and the nature of the fracture. The humerus, the long bone in the upper arm, is often fractured due to trauma like falls, which are common in older adults, particularly those with osteoporosis. While a comminuted fracture implies the bone is broken in multiple fragments, a "non-displaced" classification is crucial, meaning the bone pieces remain in their correct anatomical alignment or with minimal displacement. This significantly influences the treatment approach and, consequently, the expected recovery and functional outcome.
Key Highlights of Functional Outcome
- Non-operative treatment is often preferred: For non-displaced or minimally displaced comminuted proximal humerus fractures, especially in elderly patients, non-surgical management is frequently the initial and often successful approach.
- Good functional outcomes are achievable: Despite the complexity of a comminuted fracture, many elderly patients who undergo non-operative treatment for non-displaced proximal humerus fractures can achieve satisfactory functional results, often with acceptable levels of pain and range of motion.
- Rehabilitation adherence is critical: Consistent adherence to physiotherapy and the use of an orthosis (like a sling) are key factors in maximizing functional recovery and preventing complications, even if the patient experiences some limitations in activity or social participation.
Understanding the Fracture: Comminuted and Non-Displaced
What Does It Mean for the Humerus?
A comminuted fracture refers to a bone that is broken into three or more pieces. These types of fractures often result from high-energy trauma but can occur from simple falls in older individuals with weakened bones (osteoporosis). The term "non-displaced" is equally important. It signifies that despite the bone being broken into multiple fragments, these fragments have not significantly shifted out of their original alignment. This distinction is critical because non-displaced fractures often lend themselves well to conservative (non-surgical) management.
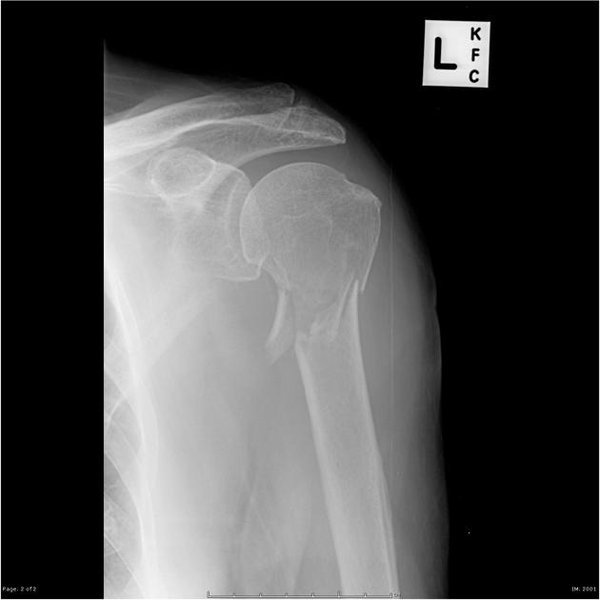
The humerus is typically divided into three main sections for fracture classification: proximal (near the shoulder), shaft (middle), and distal (near the elbow). Proximal humerus fractures are particularly common in older adults, accounting for a significant percentage of all fractures in this demographic. Given the 67-year-old woman's age, a proximal humerus fracture is a likely scenario, often resulting from a ground-level fall on an outstretched arm.
Treatment Approaches and Healing Timeline
Conservative Management as a Primary Option
For a comminuted non-displaced humeral fracture in a 67-year-old woman, conservative management is often the preferred treatment. This typically involves immobilization of the arm in a sling or shoulder immobilizer. The goal is to allow the bone to heal naturally while minimizing pain and maintaining acceptable alignment. Approximately 65% to 85% of proximal humerus fractures, especially those with minimal displacement, are successfully managed without surgery in elderly patients.
Initial Immobilization and Early Phases
In the initial phase, immobilization is crucial. A splint may be used for three to five weeks, while a cast might be needed for six to eight weeks. For non-displaced comminuted fractures, immobilization in an orthosis for about three weeks is often sufficient. During this time, the body begins the complex process of bone repair. The initial healing phase generally takes about 6-8 weeks, during which the bone fragments start to unite.
The Role of Physical Therapy
Following the immobilization period, physical therapy becomes a cornerstone of recovery. Early initiation of physical therapy, sometimes within 14 days of injury, has been shown to correlate with better functional outcomes. The rehabilitation protocol aims to regain strength and range of motion in the arm and shoulder. This is a progressive process, starting with gentle exercises and gradually advancing to more active movements and strengthening exercises. Adherence to this protocol is a significant predictor of a successful functional outcome.
Considerations for Surgical Intervention
While non-operative treatment is common for non-displaced fractures, surgery might be considered in specific cases, such as highly displaced fractures, certain complex comminuted patterns, or if conservative management fails to achieve satisfactory results. However, for elderly patients, surgical intervention carries increased risks of complications, including reintervention rates. Many studies indicate that for proximal humerus fractures in the elderly, surgery does not necessarily lead to better functional outcomes or quality of life compared to non-surgical treatment, particularly for 3- and 4-part fractures.
Expected Functional Outcomes and Influencing Factors
Achieving Acceptable Function in the Elderly
The functional outcome for a 67-year-old woman with a comminuted non-displaced humeral fracture treated non-operatively can generally be good. The primary goals of treatment are to reduce pain and regain function. While some reduction in the range of motion is common regardless of the treatment modality, most elderly patients achieve an acceptable functional result. This means they can often resume many of their daily activities with a good level of independence.
Factors Influencing Outcome
- Adherence to Rehabilitation: As mentioned, consistent engagement with physical therapy and proper use of supportive devices (like slings) is paramount. Patients who struggle with compliance may experience poorer functional outcomes.
- Bone Quality: Osteoporosis, common in elderly patients, can affect healing rates and the overall stability of the fracture during recovery.
- Patient's Pre-injury Activity Level and Expectations: A patient's prior functional demands and their personal goals for recovery play a role in defining "satisfactory" outcome. Lower-demand patients may tolerate slight limitations better.
- Associated Injuries/Comorbidities: Other medical conditions or injuries can impact the recovery process and overall functional outcome.
- Fracture Type and Severity: Although the fracture is non-displaced, the degree of comminution and specific fracture pattern can still influence the healing process and the potential for residual stiffness or pain.
Long-Term Outlook and Potential Challenges
While the humerus bone almost always heals, malunion (healing in an imperfect alignment) can occur with non-operative treatment, especially for displaced fractures. However, for non-displaced fractures, this risk is minimized, and even if some malunion occurs, it does not necessarily lead to poor function or pain in elderly patients. Stiffness in the shoulder joint is a common long-term complication after humerus fractures, regardless of treatment type. The recovery period for comminuted fractures can be extended, potentially taking a year or longer for complete healing, especially if surgery was required. However, for non-displaced fractures, the initial healing phase is typically shorter, around 6-8 weeks, with functional recovery continuing over several months.
Comparing Treatment Avenues: Operative vs. Non-Operative
A Balanced Perspective for the Elderly
For a 67-year-old woman with a non-displaced comminuted proximal humerus fracture, the literature strongly supports non-operative treatment as a viable and often superior option in terms of overall patient-reported outcomes, especially concerning health-related quality of life (HRQoL) and pain. Studies have found no significant difference in functional outcomes between operative and non-operative management for displaced 3- and 4-part proximal humerus fractures in patients aged 65 and older.
Operative treatment, while offering stable fixation and potentially earlier mobilization, is associated with considerable complication rates, particularly in osteoporotic bone. These complications can include screw penetration, infection, or failure of the fixation hardware, often necessitating further surgery. Economically, surgical treatment is significantly more expensive than non-operative care.
The following radar chart illustrates a comparative perspective on various aspects of operative versus non-operative treatment for complex proximal humerus fractures in elderly patients, based on aggregated evidence and general trends. This visualization helps highlight the nuanced trade-offs involved in treatment decisions.
Making Informed Decisions
Ultimately, the decision between operative and non-operative treatment for a comminuted non-displaced humeral fracture in an elderly patient is a shared one, involving the patient, their family, and the healthcare team. Factors such as the patient's overall health, functional demands, bone quality, and the surgeon's experience all play a role. For a 67-year-old woman with a non-displaced comminuted fracture, the emphasis is often on achieving a pain-free, functional arm that allows her to maintain independence and quality of life, which non-operative treatment frequently accomplishes without the added risks of surgery.
Comparing Different Humerus Fracture Types
Healing and Outcomes Across the Humerus
While the focus here is on a comminuted non-displaced fracture, it's helpful to understand how different types of humerus fractures might compare in terms of healing and functional outcomes, especially in the elderly population. The humerus can break in various locations: proximal (near the shoulder), shaft (middle), and distal (near the elbow). The nature of the break (e.g., transverse, oblique, spiral, segmental, impacted, or buckle) and the degree of displacement also significantly influence the prognosis.
Fracture Type/Location |
Common Treatment Approach (Elderly) |
Typical Healing Time |
Expected Functional Outcome |
Potential Complications/Considerations |
|---|---|---|---|---|
| Proximal Humerus (Non-Displaced Comminuted) | Non-operative (sling/immobilizer, early physical therapy) | 6-8 weeks for initial bone healing; several months for functional recovery. | Generally good, with acceptable pain and regained function for daily activities. Some reduction in range of motion common. | Stiffness, mild residual pain, malunion (rarely debilitating if non-displaced), potential for prolonged rehabilitation. |
| Proximal Humerus (Displaced) | Often operative (plates, screws, or arthroplasty), but non-operative is also considered. | Longer healing, 3-6 months or more for significant functional return. | Variable. Can be good, but often with more significant limitations in range of motion and higher risk of complications. | Higher risk of avascular necrosis, non-union, implant failure, stiffness, nerve injury, reoperation. |
| Humeral Shaft (Non-Displaced/Minimally Displaced) | Non-operative (functional bracing) | Approx. 10-12 weeks for bone union. | Good functional alignment and recovery in most cases. | Radial nerve palsy (common, often resolves), malunion (often well-tolerated functionally). |
| Humeral Shaft (Displaced/Comminuted) | Operative (plates, rods) or non-operative (functional bracing for selected cases). | Varies significantly; 3-6 months or more. | Good for union, but potential for nerve injury and residual weakness. | Non-union, infection, nerve injury, compartment syndrome. |
| Distal Humerus (General) | Often operative (complex fixation) due to involvement of elbow joint. Conservative treatment exceptional in elderly. | Prolonged; often a year or more for full recovery. | Satisfactory functional outcomes possible, but stiffness and reduced range of motion of the elbow are common. | Stiffness, post-traumatic arthritis, nerve injury, non-union, infection. |
Frequently Asked Questions (FAQ)
Conclusion
For a 67-year-old woman experiencing a comminuted non-displaced humeral fracture, the prognosis for a good functional outcome is favorable, particularly with non-operative management. The conservative approach, involving immobilization followed by a dedicated physical therapy regimen, is often sufficient to achieve satisfactory recovery, allowing the patient to regain substantial independence and reduce pain. While the path to full recovery can extend over several months, diligent adherence to rehabilitation protocols is paramount for optimizing mobility and minimizing long-term complications such as stiffness. The evidence suggests that for many elderly patients, non-surgical treatment offers comparable or even superior outcomes to surgery without the associated risks and costs, emphasizing a patient-centered approach that prioritizes pain relief and functional restoration tailored to individual needs and expectations.
Recommended Further Reading
- Explore detailed rehabilitation protocols for proximal humerus fractures in older adults.
- Investigate potential complications and challenges in non-operative humerus fracture management.
- Understand how osteoporosis influences bone healing in elderly patients with fractures.
- Delve into studies on the long-term quality of life experienced by elderly patients after a humerus fracture.
References
Last updated May 21, 2025