
Understanding the Conjunctiva
A comprehensive guide to the anatomy, function, and health of the eye’s protective membrane
Key Insights
- Anatomical Structure: The conjunctiva is a thin, transparent mucous membrane covering the inner eyelid and the anterior sclera, divided into distinct anatomical regions.
- Essential Functions: It plays vital roles in protection, lubrication, immune defense, and mechanical support, ensuring the eye remains healthy and comfortable.
- Common Disorders: Several ocular conditions such as conjunctivitis, conjunctivochalasis, and pterygium stem from its susceptibility to environmental, infectious, and degenerative influences.
Introduction
The conjunctiva is a critical component of the eye’s anatomy that many people overlook, yet it performs specialized functions that are pivotal for maintaining ocular health. As a thin, transparent mucous membrane, the conjunctiva not only provides protection from various environmental hazards but also plays an integral role in lubrication and immune surveillance. Its unique structure allows mobility and flexibility, facilitating smooth movement of the eyelids and contributing to the overall comfort and functionality of the eye.
Anatomy and Structure
Overview
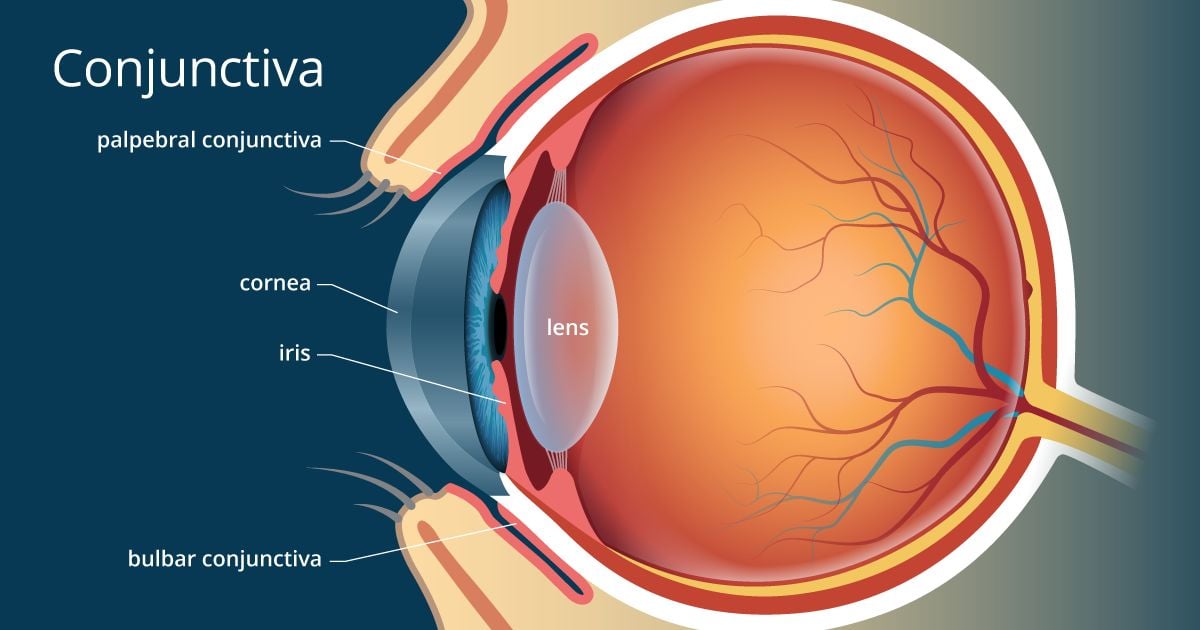
The conjunctiva is divided into multiple regions, each with distinct anatomical and histological features. The membrane extends over the inner surface of the eyelids (palpebral conjunctiva) and overlays the anterior portion of the sclera (bulbar conjunctiva). Additionally, a transitional region, known as the fornix conjunctiva, connects these two main areas and forms a cul-de-sac that facilitates tear distribution and eyelid movement.
Regional Divisions
The primary parts of the conjunctiva include:
- Palpebral Conjunctiva: Lines the inner aspect of the eyelids and is structured to allow smooth translation over the eye surface during blinking.
- Bulbar Conjunctiva: Covers the anterior part of the sclera, providing a transparent layer that supports the underlying vascular network and adds to the overall moisture of the eye.
- Fornix Conjunctiva: Represents the junctional fold between the palpebral and bulbar conjunctivas. This area forms a recessed sac that facilitates tear collection and distribution.
Histological Composition
Microscopically, the conjunctiva is composed of a non-keratinized stratified epithelium that includes:
- Epithelial Cells: Typically stratified squamous cells that vary in arrangement depending on location. In some areas, cells can appear in columnar or cuboidal shapes.
- Goblet Cells: Specialized mucus-secreting cells that produce mucins such as MUC 5AC, which are pivotal for maintaining tear film stability.
- Lamina Propria: A layer beneath the epithelium consisting of loose connective tissue enriched by blood vessels, lymphatic channels, and immune cells, providing nutritional support and mediating immune responses.
Vascularization and Innervation
One striking aspect of the conjunctiva is its rich vascularization. Numerous small blood vessels permeate the tissue, contributing to its role in thermal regulation and repair. Additionally, the conjunctiva is innervated by branches of the trigeminal nerve, which confers sensory feedback including pain, touch, temperature, and mechanical pressure.
| Region | Location | Main Functions |
|---|---|---|
| Palpebral Conjunctiva | Inner eyelid surface | Smooth eyelid motion, lubrication |
| Bulbar Conjunctiva | Anterior sclera (excluding the cornea) | Protective barrier, tear film stability, vascular supply |
| Fornix Conjunctiva | Transition zone between palpebral and bulbar regions | Tear reservoir, flexibility for eyelid movement |
Functions of the Conjunctiva
Protection and Barrier Formation
The conjunctiva serves as a frontline defender against harmful environmental agents. Its transparent, mucous membrane acts as a physical barrier, effectively shielding the eye from dust, debris, chemical irritants, and microbial pathogens. This protective measure ensures that the delicate internal structures of the eye remain undisturbed, reducing the risk of infection or injury.
Role in Immune Surveillance
Embedded within the lamina propria are several immune cells tasked with ongoing surveillance to detect and combat potential pathogens. This immune function is crucial for instantaneous local responses, helping to prevent the spread of infections. In instances where harmful microorganisms are detected, the conjunctival immune response can initiate inflammation to contain and eliminate the threat.
Lubrication and Tear Film Maintenance
Another significant responsibility of the conjunctiva is maintaining the eye’s moisture balance. The tissue secretes mucus via goblet cells and contributes to the watery component necessary for a stable and continuous tear film. This tear film not only ensures comfort by minimizing friction during blinking, but it also plays a vital role in delivering oxygen and nutrients to the eye’s surface.
Accessory Lacrimal Function
Besides the primary lacrimal gland, accessory lacrimal tissue present in the conjunctiva assists in the production of the aqueous layer of the tear film. This cooperation is essential in preventing the drying out of the ocular surface and maintaining clear, consistent vision.
Mechanical Support and Mobility
The conjunctiva provides necessary mechanical support to the eye. Its flexible, yet robust, structure allows smooth movements of the eyelid over the eye’s surface. The motion facilitated by the conjunctiva minimizes friction and shearing forces during blinking, which is integral to preserving both comfort and the integrity of the corneal surface.
Additionally, the loose connective tissue within the conjunctiva permits displacement and resilience, ensuring that minor injuries or abrasions can be effectively managed without affecting overall eye function.
Common Conditions and Disorders
Conjunctivitis
Conjunctivitis, widely known as "pink eye," is the inflammation of the conjunctiva. It may arise from several causes, including bacterial or viral infections, allergic reactions, and chemical irritants. The hallmark symptoms include redness, irritation, and discharge. In cases involving infections, the conjunctiva becomes visibly red due to the dilation of its blood vessels, a response to the invading pathogens.
Conjunctivochalasis
Conjunctivochalasis is characterized by the looseness or redundancy of the conjunctival tissue, often resulting in a wrinkled appearance. This condition is particularly common in older adults due to the natural aging process and may lead to discomfort, dryness, blurred vision, or even interference with tear distribution.
Pterygium and Pinguecula
Other ocular conditions related to the conjunctiva include pterygium and pinguecula. Pterygium involves the growth of conjunctival tissue onto the cornea. While it is usually benign, if the growth becomes extensive, it can disrupt the tear film and impair vision. On the other hand, pinguecula is a yellowish, raised lesion on the conjunctiva that emerges primarily due to prolonged sun exposure. Although generally harmless, pinguecula may be a cosmetic concern or cause minor irritation.
Other Conjunctival Disorders
In addition to the above, the conjunctiva can be affected by trauma, chemical burns, or systemic inflammatory conditions. In all instances, prompt diagnosis and treatment are essential to prevent complications and maintain ocular health. Detailed eye examinations often include assessments of the conjunctiva’s health, and treatment may range from the use of lubricating eye drops to more specialized medical or surgical interventions.
Diagnostic and Therapeutic Innovations
Modern Diagnostic Techniques
Advances in ocular imaging and diagnostic technologies have enabled clinicians to closely evaluate the conjunctiva. Techniques such as slit-lamp biomicroscopy allow for the detailed inspection of the mucous membrane’s microscopic features, vascular patterns, and structural integrity. Moreover, high-resolution imaging can detect subtle changes that may indicate early signs of inflammation, neoplasia, or degenerative changes.
Imaging and Histological Examination
In many cases, when abnormalities are suspected, doctors may employ in vivo confocal microscopy or perform conjunctival biopsies. These methods help in distinguishing benign lesions from conditions with a potential for malignancy, thus guiding appropriate intervention.
Therapeutic Strategies
Treatment modalities for conjunctival disorders vary widely, ranging from conservative management with eye drops and lubricants to surgical procedures for more severe cases. For example, bacterial conjunctivitis is frequently treated with antibiotic eye drops, while allergic forms are managed with antihistamines and corticosteroids. More advanced surgical techniques may be necessary for conditions such as pterygium, ensuring removal of the aberrant tissue and preventing recurrence. Furthermore, ongoing research in regenerative medicine and immunomodulation holds promise for new treatments that can more effectively restore the health of the conjunctival tissue.
The Conjunctiva in Systemic Health
Role in Immune and Inflammatory Responses
Beyond its localized functions, the conjunctiva plays a role in the systemic health of individuals. Due to its constant exposure to environmental agents, it not only acts as a first line of immune defense but can also serve as an indicator of systemic conditions. Inflammatory diseases, autoimmune disorders, and even nutritional deficiencies may manifest through changes in the appearance and function of the conjunctiva.
Monitoring and Preventive Health Measures
Regular ophthalmologic examinations often include an assessment of the conjunctiva. This is important not only in diagnosing ocular conditions but also in identifying early signs of systemic diseases. Preventive measures such as the use of protective eyewear, avoidance of excessive UV exposure, and adherence to good hygiene practices are instrumental in preserving both the conjunctiva and overall eye health.
Emerging Research Directions
Cellular and Molecular Insights
Ongoing research into the cellular and molecular makeup of the conjunctiva is expanding our understanding of its functions and potential therapeutic targets. Recent studies focus on the role of goblet cells and the specific mucins they produce, which are essential in preserving the tear film. Research is also directed toward understanding the regenerative capabilities of conjunctival cells, potentially paving the way for novel treatments for severe ocular surface injuries.
Innovative Treatments and Regeneration
Investigators are exploring regenerative medicine techniques, such as the use of stem cells, to promote the repair and regeneration of damaged conjunctival tissue. This field of study holds promise for patients with chronic inflammatory conditions or those who have suffered trauma, ultimately aiming for restored functionality and improved quality of life.
Interdisciplinary Approaches
The study of the conjunctiva increasingly benefits from interdisciplinary collaboration, integrating insights from immunology, cellular biology, and advanced medical imaging. Such collaborative efforts are leading to a more holistic understanding of ocular health and are guiding the development of integrated treatment protocols that address both local ocular issues and systemic health factors.
References
- Conjunctiva - Wikipedia - Wikipedia
- Conjunctiva: Eye Anatomy - All About Vision
- Conjunctiva Anatomy - Kenhub
-
Conjunctiva: Function & Common Conditions - Cleveland Clinic
- Conjunctiva - MedlinePlus
- Understanding Your Conjunctiva - Verywell Health
- Conjunctiva Overview - Oscar Wylee
-
Eye Anatomy Overview - All About Vision
-
The Conjunctiva: Histology and Function - NCBI
- Conjunctiva Details - American Academy of Ophthalmology
Recommended Queries for Further Exploration
Last updated March 1, 2025