
Unlocking Relief: Your Comprehensive Guide to Managing Spinal Osteophyte Pain
Discover effective strategies, from lifestyle adjustments to advanced treatments, to alleviate discomfort from bone spurs.
Spinal osteophytes, commonly known as bone spurs, are smooth, bony growths that typically form along the edges of vertebrae. While many individuals with osteophytes experience no symptoms, these growths can lead to significant pain and discomfort if they impinge on nearby nerves, restrict movement in the spinal canal, or cause inflammation in the joints. Understanding how to manage this pain is crucial for maintaining quality of life. This guide offers a comprehensive overview of current strategies, blending insights from multiple medical perspectives as of May 21, 2025.
Key Insights into Managing Spinal Osteophyte Pain
- Prioritize Conservative Care: Most spinal osteophyte pain can be managed effectively through non-surgical methods like medication, physical therapy, and lifestyle changes. These approaches aim to reduce inflammation, alleviate pressure, and improve spinal function.
- Understand the "Why": Pain typically arises not from the bone spur itself (which is often smooth), but when it compresses spinal nerves (radiculopathy), the spinal cord (myelopathy), causes friction between vertebrae, or leads to inflammation and stiffness.
- Personalized Approach is Key: Effective management requires a tailored treatment plan developed in consultation with healthcare professionals, such as a neurologist, orthopedist, or spine specialist. The plan will consider the specific location (cervical, thoracic, lumbar), size, and symptomatic impact of your osteophytes.
Decoding Spinal Osteophytes and Their Impact
What Are Spinal Osteophytes and Why Do They Cause Pain?
Spinal osteophytes are often a consequence of the body's response to ongoing wear and tear, typically associated with aging, osteoarthritis, degenerative disc disease, or past spinal injuries. As cartilage in the spinal joints deteriorates, the body may attempt to stabilize the affected area by forming these bony projections.
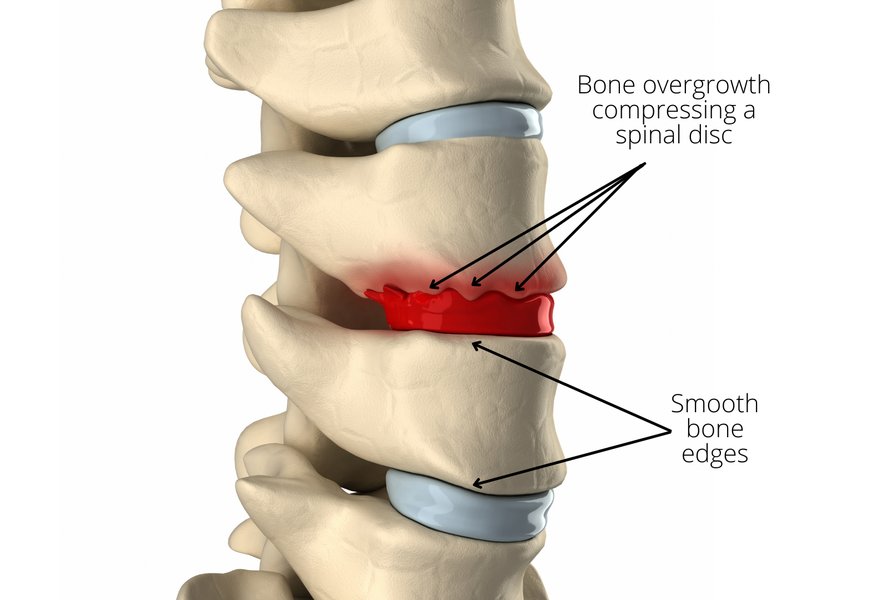
Anatomical illustration showing osteophytes (bone spurs) on spinal vertebrae.
The pain and other symptoms associated with spinal osteophytes emerge when these growths:
- Compress Nerve Roots: Osteophytes can narrow the neural foramina, the openings through which nerve roots exit the spinal column. This can lead to radiculopathy, characterized by pain, numbness, tingling (paresthesia), or weakness that radiates into the arms or legs, depending on the location of the spur (e.g., cervical osteophytes affect arms, lumbar osteophytes affect legs).
- Compress the Spinal Cord: In more severe instances, osteophytes can grow into the spinal canal, reducing space for the spinal cord. This condition, known as myelopathy, can cause more serious symptoms like widespread weakness, balance problems, loss of coordination, and bowel or bladder dysfunction.
- Cause Joint Inflammation and Friction: Bone spurs on the facet joints (the small stabilizing joints located between and behind adjacent vertebrae) can cause vertebrae to rub against each other, leading to inflammation, pain, and stiffness, particularly with movement like bending or twisting.
- Restrict Range of Motion: The presence of osteophytes can limit the spine's natural flexibility, leading to stiffness and pain, especially during or after activity.
Factors contributing to osteophyte development include aging, osteoarthritis, repetitive strain, poor posture, genetic predisposition, and excess body weight. Early and accurate diagnosis is crucial for effective pain management.
Non-Surgical Pain Management Strategies: The First Line of Defense
For most individuals, pain from spinal osteophytes can be effectively managed with conservative, non-surgical treatments. The primary goals are to reduce inflammation, alleviate pain, improve spinal mechanics, and strengthen supporting musculature. These methods are typically explored for several weeks to months before considering more invasive options.
Medications for Pain and Inflammation Control
Over-the-Counter (OTC) Options
Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) and naproxen sodium (Aleve) are commonly recommended to reduce both pain and inflammation. Acetaminophen (Tylenol) can help with pain relief but does not have significant anti-inflammatory properties.
Prescription Medications
If OTC medications are insufficient, your doctor might prescribe stronger anti-inflammatory drugs, muscle relaxants to ease associated muscle spasms, or other types of pain relievers. It's common for physicians to reassess the effectiveness of new medications within 4 to 6 weeks.
Physical Therapy: Restoring Function and Strength
Physical therapy is a cornerstone of managing osteophyte-related pain. A qualified physical therapist will design a tailored program focusing on:
- Strengthening Exercises: Targeting core, back, and abdominal muscles to provide better spinal support and reduce pressure on affected joints.
- Flexibility and Range-of-Motion Exercises: Gentle stretches to alleviate stiffness, improve mobility, and decompress spinal structures.
- Postural Education and Ergonomics: Learning how to maintain proper posture during daily activities (sitting, standing, lifting) to minimize spinal strain.
- Manual Therapy: Techniques such as massage or joint mobilization performed by the therapist to reduce pain and improve movement.
Lifestyle Modifications: Empowering Self-Care
Weight Management
Excess body weight significantly increases the load on spinal joints. Losing even a modest amount of weight can noticeably reduce stress on the spine, particularly in the lumbar region, and alleviate pain.
Activity Modification and Strategic Rest
Avoiding activities that exacerbate pain, such as heavy lifting, prolonged bending, or high-impact sports, is crucial. Strategic rest during acute flare-ups can help, but complete inactivity should be avoided to prevent further stiffness. Some individuals find relief when leaning forward or bending at the waist, as this can temporarily decompress the spinal canal.
Proper Posture and Ergonomics
Consciously maintaining good posture while sitting (e.g., upright with frequent breaks), standing, and sleeping can help alleviate undue pressure on the spine and prevent further irritation of osteophytes.
Heat and Ice Therapy: Simple Yet Effective Relief
Applying heat or ice can provide symptomatic relief:
- Ice Therapy: Applying ice packs (wrapped in a cloth) for 15-20 minutes can help reduce acute inflammation, swelling, and numb painful areas, especially after a flare-up or strenuous activity.
- Heat Therapy: Warm showers, heating pads, or heated gel packs can help relax tense muscles, ease chronic stiffness, and improve blood flow to the affected area.
Injection Therapies: Targeted Anti-Inflammatory Action
When pain is persistent or involves significant nerve irritation, injections can offer relief:
- Corticosteroid Injections: Epidural steroid injections or local corticosteroid injections administered near the affected nerve root or facet joint can significantly reduce inflammation and pain. These are typically performed under fluoroscopic (X-ray) guidance to ensure precise placement. While effective for many, the relief is often temporary, and injections are generally limited to a few per year in any single joint to avoid potential side effects like tissue weakening or systemic effects.
- Local Anesthetic Injections: Sometimes combined with corticosteroids, local anesthetics can provide immediate, short-term pain relief.
These injections can provide a window of pain relief that allows patients to more effectively participate in physical therapy and rehabilitation programs.
Comparative Efficacy of Non-Surgical Treatments
The following chart provides a general comparison of various non-surgical treatment modalities for spinal osteophyte pain based on common clinical observations. The effectiveness and suitability of each can vary greatly among individuals.
Complementary and Integrative Therapies
Some individuals find additional relief with therapies such as:
- Massage Therapy: Can help relieve muscle tension, improve circulation, and reduce pain.
- Acupuncture: Involves inserting fine needles into specific points on the body, which some find effective for pain relief.
- Chiropractic Adjustments: Manual manipulation of the spine by a qualified chiropractor may improve spinal alignment and mobility, potentially reducing symptoms for some patients. However, this approach is not suitable for everyone and should be discussed with a doctor.
- Traction: Mechanical or manual traction can sometimes be used to gently stretch the spine and relieve pressure on nerves.
Visualizing Treatment Pathways for Spinal Osteophytes
The journey to managing spinal osteophyte pain often involves several stages, from initial diagnosis to exploring various treatment modalities. The mindmap below illustrates a typical progression and the interconnectedness of different management strategies.
(Bony growths on vertebrae)"] id1b["Why they cause pain?
(Nerve/cord compression, Inflammation, Restricted movement)"] id2["Non-Surgical Treatments (First-Line)"] id2a["Medications
(NSAIDs, Acetaminophen, Muscle Relaxants)"] id2b["Physical Therapy
(Strengthening, Flexibility, Posture Correction)"] id2c["Lifestyle Modifications
(Weight Management, Activity Adjustment, Ergonomics)"] id2d["Heat & Ice Therapy
(Symptomatic relief)"] id2e["Injections
(Corticosteroids for inflammation)"] id2f["Complementary Therapies
(Massage, Acupuncture, Chiropractic - with caution)"] id3["Evaluation & Monitoring"] id3a["Regular follow-up with healthcare provider"] id3b["Assessment of symptom improvement"] id4["Surgical Interventions (Considered if conservative care fails or severe compression)"] id4a["When to Consider?"] id4aa["Persistent debilitating pain (e.g., >3-6 months)"] id4ab["Progressive neurological deficits (weakness, numbness)"] id4ac["Significant spinal cord compression (myelopathy)"] id4ad["Severe spinal stenosis"] id4b["Common Surgical Procedures"] id4ba["Osteophyte Resection (Direct removal of bone spur)"] id4bb["Laminectomy/Laminotomy (Decompressing spinal canal/nerves)"] id4bc["Spinal Decompression (General term)"] id4bd["Anterior Cervical Discectomy and Fusion (ACDF)"] id4be["Minimally Invasive Surgery (MIS) options"] id5["Post-Treatment & Long-Term Management"] id5a["Post-operative rehabilitation (if surgery performed)"] id5b["Ongoing lifestyle management"] id5c["Continued exercises and posture awareness"]
Surgical Interventions: When Conservative Measures Aren't Enough
Surgery is generally considered a last resort, reserved for cases where non-surgical treatments have failed to provide adequate relief after an extended period (typically three to six months or more), or when there is significant neurological compromise.
When is Surgery Recommended?
Key indications for surgical consideration include:
- Persistent, severe pain that significantly impacts daily life and doesn't respond to conservative care.
- Progressive neurological symptoms such as increasing numbness, weakness in the limbs, or loss of motor/sensory function.
- Evidence of spinal cord compression (myelopathy) or severe spinal stenosis (narrowing of the spinal canal) caused by osteophytes.
- Bowel or bladder dysfunction (a rare but serious symptom requiring urgent attention).
Common Surgical Procedures for Spinal Osteophytes
The goal of surgery is typically to decompress the affected nerves or spinal cord by removing the problematic bone spurs or creating more space within the spinal canal.
Osteophyte Resection
This procedure involves the direct surgical removal of the bone spurs that are impinging on nerves or other spinal structures. It is often performed in conjunction with other decompressive surgeries.
Laminectomy or Laminotomy
A laminectomy involves removing a portion of the lamina (the bony arch at the back of a vertebra) to create more space in the spinal canal, relieving pressure on the spinal cord or nerve roots. A laminotomy is a less extensive procedure where only a small part of the lamina is removed.
Spinal Decompression Surgery
This is a broader term encompassing various procedures designed to alleviate pressure on the spinal cord or nerves. The specific type depends on the location and nature of the compression. Examples include foraminotomy (enlarging the neural foramen) or discectomy (removing a problematic intervertebral disc that may be contributing to nerve compression alongside osteophytes).
Anterior Cervical Discectomy and Fusion (ACDF)
For cervical osteophytes causing significant nerve root compression or spinal cord issues, ACDF may be performed. This involves removing the damaged disc and any associated bone spurs from the front of the neck, then fusing the adjacent vertebrae to provide stability.
Minimally Invasive Surgery (MIS) Techniques
Whenever possible, surgeons may opt for minimally invasive approaches. These techniques use smaller incisions and specialized instruments, often leading to less post-operative pain, shorter hospital stays, and faster recovery times compared to traditional open surgery.
Post-surgery, a period of rehabilitation, often including physical therapy, is essential to regain strength, flexibility, and full function. Recovery times vary based on the type of surgery and individual factors.
Understanding Spinal Osteophytes Through Video
For a visual explanation of what spinal bone spurs are and an overview of how they can affect the spine, the following video provides valuable insights. It discusses the nature of osteophytes and touches upon general treatment considerations.
This video offers a general overview of spinal bone spurs (osteophytes) and their treatment considerations.
Comparative Overview of Pain Management Strategies
Choosing the right pain management strategy for spinal osteophytes depends on various factors including the severity of symptoms, location of the osteophytes, overall health, and personal preferences. Below is a table summarizing key non-surgical approaches:
| Treatment Modality | Primary Mechanism of Action | Key Benefits | Common Considerations / Potential Side Effects |
|---|---|---|---|
| Medications (e.g., NSAIDs, Acetaminophen) | Reduce inflammation (NSAIDs), block pain signals | Rapid pain and/or swelling reduction | GI upset, cardiovascular risks (long-term NSAID use), kidney issues; Acetaminophen lacks anti-inflammatory effect. |
| Physical Therapy | Strengthens supporting muscles, improves flexibility, posture, and spinal mechanics | Improved function, reduced nerve pressure, long-term relief, patient education | Requires commitment and active participation, initial discomfort possible during exercises. |
| Lifestyle Modifications (Weight, Activity, Posture) | Reduces mechanical stress on the spine, minimizes irritation | Sustainable pain reduction, overall health improvement, empowers self-management | Requires consistent effort and behavior change, may involve activity limitations. |
| Heat & Ice Therapy | Ice reduces acute inflammation/swelling; Heat relaxes muscles, improves blood flow | Symptomatic relief, easy to apply at home, non-invasive | Primarily temporary relief, risk of skin irritation if not used properly. |
| Corticosteroid Injections | Potent anti-inflammatory effect delivered directly to the source of pain/inflammation | Significant, often rapid pain relief for flare-ups, can facilitate physical therapy | Relief often temporary, potential for infection, nerve damage (rare), limited number of injections advisable, possible systemic effects. |
| Complementary Therapies (Massage, Acupuncture, etc.) | Varies (e.g., improved circulation, muscle relaxation, nerve modulation, endorphin release) | Holistic pain management, stress reduction, may improve overall well-being | Effectiveness varies by individual and therapy type, crucial to choose qualified and licensed practitioners. |
Frequently Asked Questions (FAQ)
Conclusion: A Path Towards Managing Spinal Osteophyte Pain
Managing pain from spinal osteophytes is a journey that often begins with conservative, non-invasive treatments. A multifaceted approach, incorporating medications for symptom relief, physical therapy to restore function and strength, and thoughtful lifestyle adjustments, forms the foundation of effective care. For individuals whose pain persists or who experience significant neurological symptoms, targeted injections or surgical interventions may offer substantial relief. Open communication with your healthcare team is paramount to developing a personalized treatment plan that addresses your specific needs, aiming to reduce pain, improve mobility, and enhance your overall quality of life. Remember, while osteophytes themselves may be a chronic condition, the pain they cause is often manageable with the right strategies.
Recommended Further Exploration
To deepen your understanding, consider exploring these related topics:
- What are the specific physical therapy exercises recommended for lumbar osteophytes?
- How does spinal stenosis relate to osteophyte formation and pain?
- What are the long-term outcomes of surgical treatment for cervical osteophytes?
- Can diet and nutrition play a role in managing inflammation associated with spinal osteophytes?
References
Last updated May 21, 2025